Tubal Reversal Surgery
For years, tubal ligations have been a popular method of birth control for women who desired permanent sterilization. Women often describe their tubes as being tied, cut, clipped, and/or burned.
Most women who choose tubal sterilization are happy with their choice, but some women will regret the decision in years to come or have a change in their life that prompts the desire for additional children.
Women at greatest risk for regret are those who had their tubes tied before age 29, who were in an unstable relationship, those who felt pressured to have their tubes tied, and those who made the decision immediately following a pregnancy with a bad outcome.
Tubal ligation is regarded as permanent sterilization; however, in some cases it is reversible.
Can my tubes be put back together?
The procedure to reverse a tubal ligation is called a tubal reanastamosis. Whether or not you get pregnant depends on several factors. The most important factors are:
-
- method of the tubal ligation
- age of the woman
- reproductive history and/or sperm count of the man
- whether the woman ovulates or can be made to ovulate
If the ends of the fallopian tubes have been removed, the chance of successful surgery to repair the tubes is low. Similarly, if the tubes have been burned, the chance is lower.
If a large section of the tube has been removed, the reversal is not likely to be successful.
If you have any of these factors or you are 35 years old, or greater, you probably will have more success with in vitro fertilization.
Tubal Ligation Reversal vs. In Vitro Fertilization
There are many factors that determine the best method for a woman to get pregnant after she’s had her tubes tied.
Is IVF for You?
What information is needed to determine if I am a good candidate?
To determine the chance of success, we require:
-
- Semen analysis of the male partner
- Day three FSH and Estradiol, and possible clomiphene citrate challenge test (CCCT)
- The operative report documenting the details of your previous sterilization procedure.
- Proof of ovulation (serum progesterone)
How does tubal reversal surgery work?
The tubal reanastomosis procedure is generally performed as outpatient surgery, taking about two hours. An incision is made on the lower abdomen, just above the bikini line. The surgery is performed with the assistance of a microscope, using delicate techniques and sutures.
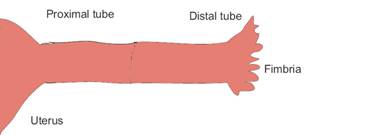
At the start of surgery, the proximal (near) and distal (far) ends are still sealed shut, as shown below.
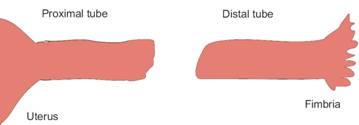
The proximal end is opened, exposing the lumen. (The lumen is the hollow part of the tube through which the egg travels to the uterus.) Dye is run through the tube to make sure the tube is now open. Then the distal end is opened.
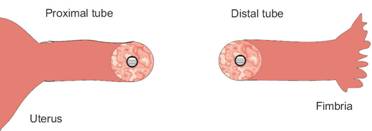
The proximal and distal lumens are then sewn together.
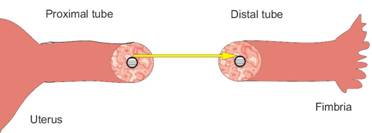
When the lumens are sewn, the outer part of the tube (serosa) is still open and will be sewn together in a separate layer. The tube is now visibly shorter.
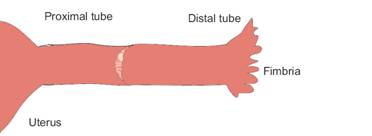
At the end of the surgery, there is only a small seam visible. Dye is run through one last time to assure that the tube is still not blocked.
How long will I be out of work?
Expected recovery time is three to four weeks, but if your job is not physically demanding, you may be able to return to work within two weeks.
What are the risks of this surgery?
The complication rate is low. All surgeries have inherent risks of bleeding, infection and damage to nearby organs, which in this case involves possibilities of the bladder, bowel, uterus, ovaries, blood vessels and nerves. However, these complications are extremely rare in this surgery.
The biggest risk is that the surgery will be unsuccessful, despite meticulous surgical technique. The chance of this depends on the type of sterilization previously performed and the condition of the fallopian tubes at the time of surgery.
It is possible that surgery will reveal other pathology, such as preexisting scar tissue, which makes the reversal more likely to fail. Furthermore, at the end of surgery the tubes may be open, but scarring can develop within the tube as it heals, resulting in a blockage.
Finally, even when the procedure is successful, it is possible the couple still has difficult conceiving despite open fallopian tubes, due to other infertility conditions that develop. While we try to minimize this risk by recommending fertility screening prior to a tubal reversal, it is impossible to eliminate this risk.
Another risk is the chance that a future pregnancy would be a tubal pregnancy (ectopic). Approximately one in 12 pregnancies after tubal reversal are ectopic. Tubal pregnancies can threaten the life of the mother if undiagnosed and untreated.
Any woman with a history of tubal surgery needs to be monitored closely until the pregnancy is seen within the uterus. By comparison, IVF has less than a 1 in 100 ectopic rate.
What is the success rate?
In properly selected patients, there is 70-80 percent chance of pregnancy within one year after the surgery.
When should I be concerned that the reversal has failed?
If you have not conceived in six months, we recommend a hysterosalpingogram (HSG) to see if the tubes are still open.
How much does tubal reanastomosis cost?
The cost of the surgery with hospital charges are approximately $8000 to $10000. You should also factor in the costs of all the testing required, usually $500 to $800. Insurance may defray the cost of testing substantially.
What are the alternatives?
If you are at high risk of the surgery failing, if the surgery does fail, or if you want to keep your tubes tied but still desire another child, then in vitro fertilization (IVF) is an excellent alternative.

